This article is part of the National Commission on Climate and Workforce Health’s series “Climate Prescription.”
Written by Dr. Leah B. Topper, a family medicine physician and Climate & Health Science Policy Fellow at the University of Colorado School of Medicine, the series translates the latest research on climate-driven health risks into practical insights for employers, HR leaders, and workplace health professionals.

At the recent Our Planet, Our Health Convention,* our workshop, 'Climate-Informed Occupational Health: Integrating Climate Risks into Workplace Clinical Encounters,' brought together 30 participants from the health care, public health, and private sectors to explore how we can incorporate climate risks into workplace-based worker health conversations.

I helped facilitate the workshop alongside Dr. Manijeh Berenji (UC Irvine Occupational and Environmental Medicine), David Leathers (Health Action Alliance), and Dr. Harleen Marwah (Mass General Brigham/Harvard Medical School).
The workshop centered on four case-based discussions designed to reflect realistic worker health situations. Participants split into small groups to identify how climate factors could increase employee health risk, determine what questions a clinician might ask, and consider both individual guidance and organizational solutions.
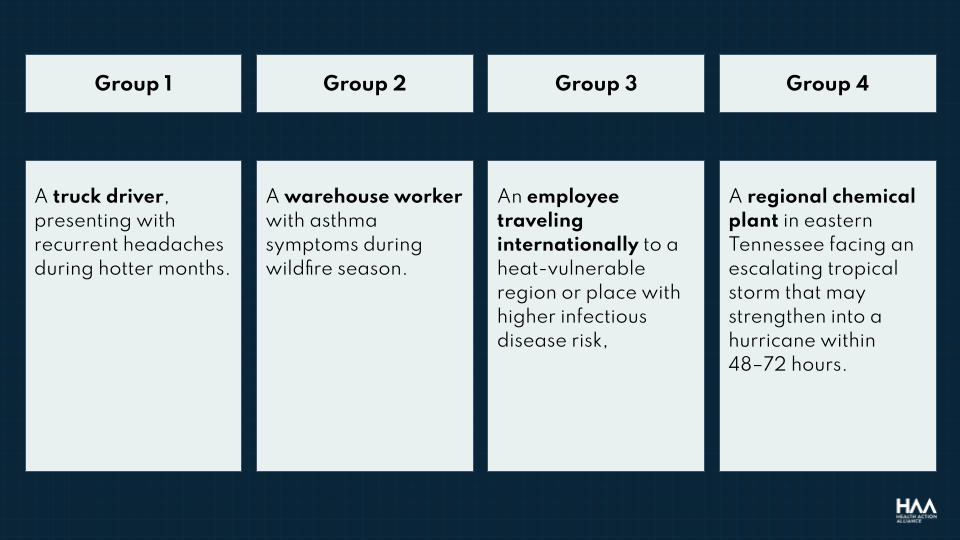
Several common themes emerged during the discussion.
First, participants expressed concerns regarding the fragmentation of care between occupational health, primary care, and specialty care clinicians, which may limit the ability to coordinate clinical care when climate risks affect workers. For example, a worker exposed to extreme heat may benefit from a decreased dose of particular blood pressure medications — but which of their clinicians is responsible for counseling them on this?
Second, the discussion highlighted the tension between individual-level recommendations and system-level interventions. While clinicians can advise workers on hydration, personal protection equipment, or medications, the most effective protections often require workplace policies such as modified schedules during extreme heat or protections implemented during high air quality index (AQI) days. Could there be a system in place where specific workplace protections are automatically implemented based on the AQI or wet bulb temperature?
Another creative idea mentioned during the workshop was a personalized risk communication tool, such as a wallet card or mobile app, that could help workers understand how their chronic health conditions interact with climate risks. It could provide specific guidance to support health-related decision-making during heat waves, wildfire events, or other environmental exposures.
Third, participants identified the need for more education. Who is responsible for educating clinicians, employers, and workers about climate-related occupational risks? Occupational health clinicians complete formal training, but not every employee has access to an occupational health provider. Furthermore, many employers are not aware of the health implications of climate exposures and thus may not know when to ask for help. Coordinated education across sectors would help address these gaps.
Finally, the discussion identified the importance of planning before, during, and after extreme climate events, with systems that triage and support the most vulnerable workers complemented by cross-sector collaborations after events to strengthen future responses.
The workshop highlighted both the growing need and the growing interest in integrating climate considerations into clinical care at the workplace. The energy and engagement from participants across disciplines were inspiring.
Our conversations reflected a recognition that protecting workers’ health in a climate-changed world requires collaboration between clinicians, employers, public health professionals, and policymakers. We must ensure that workers are protected from traditional occupational hazards and from the health risks amplified by climate change.
The challenge now is to take these conversations beyond the workshop setting and continue to translate them into real-world practice.


*Editorial note: The workshop, 'Climate-Informed Occupational Health: Integrating Climate Risks into Workplace Clinical Encounters,' was organized by the Medical Society Consortium on Climate and Health in collaboration with the National Commission on Climate and Workforce Health and Bristol Myers Squibb.
Sign up for our newsletter to keep updated on HAA’s latest initiatives, insights and recommendations, and be first to receive new resources and event invitations.
Sign up